This transcript has been edited for clarity.
Welcome to Impact Factor, your weekly dose of commentary on a new medical study. I'm Dr F. Perry Wilson of the Yale School of Medicine.
As some of you may know, I do a fair amount of clinical research developing and evaluating artificial intelligence (AI) models, particularly machine learning algorithms that predict certain outcomes.
A thorny issue that comes up as algorithms have gotten more complicated is "explainability." The problem is that AI can be a black box. Even if you have a model that is very accurate at predicting death, clinicians don't trust it unless you can explain how it makes its predictions — how it works. "It just works" is not good enough to build trust.
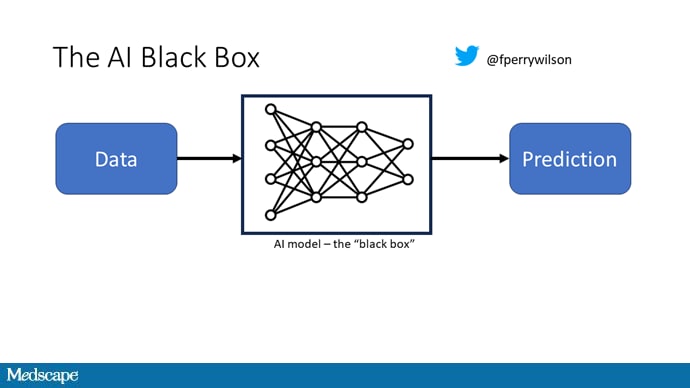
It's easier to build trust when you're talking about a medication rather than a computer program. When a new blood pressure drug comes out that lowers blood pressure, importantly, we know why it lowers blood pressure. Every drug has a mechanism of action and, for most of the drugs in our arsenal, we know what that mechanism is.
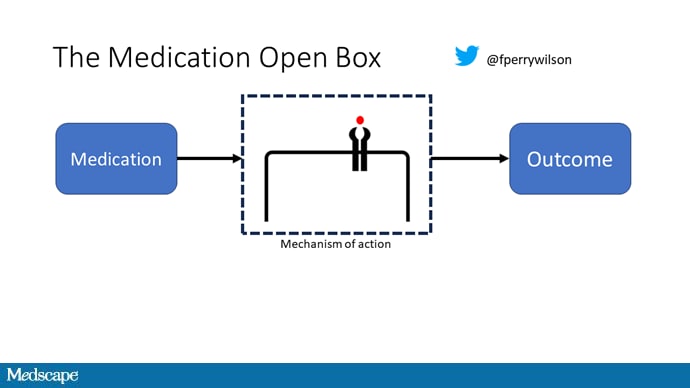
But what if there were a drug — or better yet, a treatment — that worked? And I can honestly say we have no idea how it works. That's what came across my desk today in what I believe is the largest, most rigorous trial of a traditional Chinese medication in history.
"Traditional Chinese medicine" is an omnibus term that refers to a class of therapies and health practices that are fundamentally different from how we practice medicine in the West.
It's a highly personalized practice, with practitioners using often esoteric means to choose what substance to give what patient. That personalization makes traditional Chinese medicine nearly impossible to study in the typical randomized trial framework because treatments are not chosen solely on the basis of disease states.
The lack of scientific rigor in traditional Chinese medicine means that it is rife with practices and beliefs that can legitimately be called pseudoscience. As a nephrologist who has treated someone for "Chinese herb nephropathy," I can tell you that some of the practices may be actively harmful.
But that doesn't mean there is nothing there. I do not subscribe to the "argument from antiquity" — the idea that because something has been done for a long time it must be correct. But at the same time, traditional and non–science-based medicine practices could still identify therapies that work.
And with that, let me introduce you to Tongxinluo. Tongxinluo literally means "to open the network of the heart," and it is a substance that has been used for centuries by traditional Chinese medicine practitioners to treat angina but was approved by the Chinese state medicine agency for use in 1996.
Today we'll review a large randomized trial of Tongxinluo for the treatment of ST-elevation myocardial infarction (MI), appearing in JAMA.
Like many traditional Chinese medicine preparations, Tongxinluo is not a single chemical — far from it. It is a powder made from a variety of plant and insect parts, as you can see here.
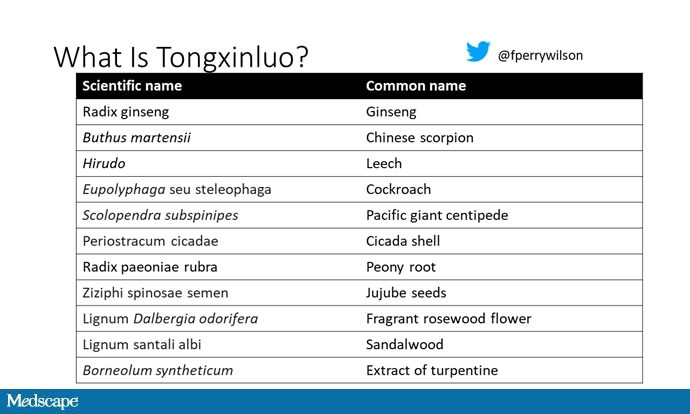
I can't imagine running a trial of this concoction in the United States; I just don't see an institutional review board signing off, given the ingredient list.
But let's set that aside and talk about the study itself.
While I don't have access to any primary data, the writeup of the study suggests that it was highly rigorous. Chinese researchers randomized 3797 patients with ST-elevation MI to take Tongxinluo — four capsules, three times a day for 12 months — or matching placebo. The placebo was designed to look just like the Tongxinluo capsules and, if the capsules were opened, to smell like them as well.
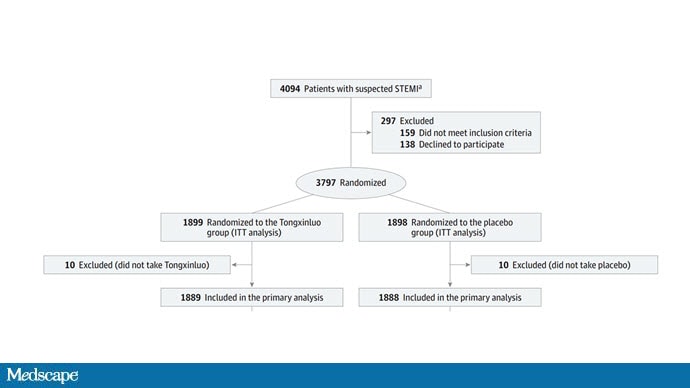
Researchers and participants were blinded, and the statistical analysis was done both by the primary team and an independent research agency, also in China.
And the results were pretty good. The primary outcome, 30-day major cardiovascular and cerebral events, were significantly lower in the intervention group than in the placebo group.
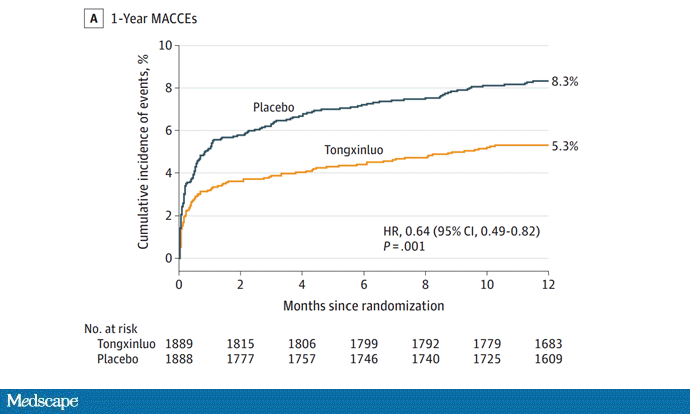
One-year outcomes were similarly good; 8.3% of the placebo group suffered a major cardiovascular or cerebral event in that timeframe, compared with 5.3% of the Tongxinluo group. In short, if this were a pure chemical compound from a major pharmaceutical company, well, you might be seeing a new treatment for heart attack — and a boost in stock price.
But there are some issues here, generalizability being a big one. This study was done entirely in China, so its applicability to a more diverse population is unclear. Moreover, the quality of post-MI care in this study is quite a bit worse than what we'd see here in the United States, with just over 50% of patients being discharged on a beta-blocker, for example.
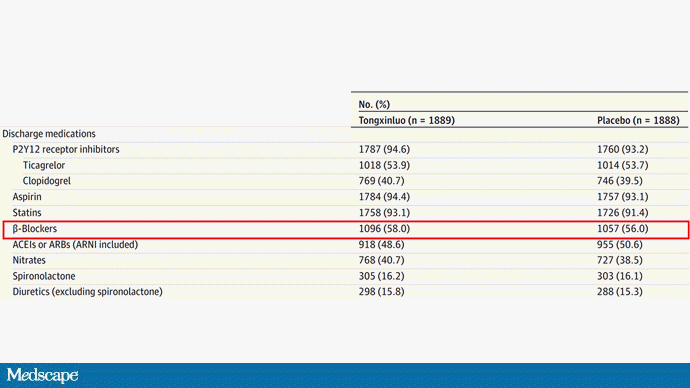
But issues of generalizability and potentially substandard supplementary treatments are the usual reasons we worry about new medication trials. And those concerns seem to pale before the big one I have here which is, you know — we don't know why this works.
Is it the extract of leech in the preparation perhaps thinning the blood a bit? Or is it the antioxidants in the ginseng, or something from the Pacific centipede or the sandalwood?
This trial doesn't read to me as a vindication of traditional Chinese medicine but rather as an example of missed opportunity. More rigorous scientific study over the centuries that Tongxinluo has been used could have identified one, or perhaps more, compounds with strong therapeutic potential.
Purity of medical substances is incredibly important. Pure substances have predictable effects and side effects. Pure substances interact with other treatments we give patients in predictable ways. Pure substances can be quantified for purity by third parties, they can be manufactured according to accepted standards, and they can be assessed for adulteration. In short, pure substances pose less risk.
Now, I know that may come off as particularly sterile. Some people will feel that a "natural" substance has some inherent benefit over pure compounds. And, of course, there is something soothing about imagining a traditional preparation handed down over centuries, being prepared with care by a single practitioner, in contrast to the sterile industrial processes of a for-profit pharmaceutical company. I get it. But natural is not the same as safe. I am glad I have access to purified aspirin and don't have to chew willow bark. I like my pure penicillin and am glad I don't have to make a mold slurry to treat a bacterial infection.
I applaud the researchers for subjecting Tongxinluo to the rigor of a well-designed trial. They have generated data that are incredibly exciting, but not because we have a new treatment for ST-elevation MI on our hands; it's because we have a map to a new treatment. The next big thing in heart attack care is not the mixture that is Tongxinluo, but it might be in the mixture.
F. Perry Wilson, MD, MSCE, is an associate professor of medicine and public health and director of Yale's Clinical and Translational Research Accelerator. His science communication work can be found in the Huffington Post, on NPR, and here on Medscape. He tweets @fperrywilson and his new book, How Medicine Works and When It Doesn't, is available now.
Follow Medscape on Facebook, X (formerly known as Twitter), Instagram, and YouTube
"hear" - Google News
October 24, 2023 at 10:20PM
https://ift.tt/SO2zj6P
This Drug Works, but Wait Till You Hear What's in It - Medscape
"hear" - Google News
https://ift.tt/kgsDpqz
https://ift.tt/d8b94jt
Bagikan Berita Ini














0 Response to "This Drug Works, but Wait Till You Hear What's in It - Medscape"
Post a Comment